Vision
Every child in Africa will receive the best supportive care to be cured from cancer.
 |
 |
|
| www.fondation-sanofi-espoir.com | ww.siop-online.org |
About
SUCCOUR – Supportive Care for Children with Cancer in Africa is one of the three projects of CANCaRe Africa, the Collaborative African Network for Children with Cancer in Africa. The vision of SUCCOUR is that every child in Africa will receive the best supportive care to be cured from cancer.
Participating centres are from Ghana, Zimbabwe, Kenya, Malawi, Ethiopia and Cameroon as shown below.
Countries of currently participating centres
SUCCOUR is a comprehensive programme aiming to improve supportive care in participating centres. The programme is building upon the Wilms Africa project and the established regional multi-disciplinary network. Local capacity building is an important element. Other components and objectives include a nursing component, educational activities, collecting locally relevant data to create and evaluate local care pathways for supportive care and the impact of our interventions. The various components of the project are shown below.
We started in 2019 with a baseline assessment of current practices and outcome in supportive care and an educational programme for nurses, recognising and appreciating the essential role of nurses in supportive care.
Leadership
Succour is currently led by Dr Trijn Israels (Blantyre, Malawi), Chair, Dr Glenn Mbah Afungchwi (Mbingo, Cameroon), Deputy-Chair and Cecilia Mdoka (Blantyre, Malawi), Central data manager. Prof Lillian Sung (Toronto, Canada), expert in supportive care and previously chair of the Scientific Committee of SIOP is an advisor.
SUCCOUR - Baseline assessment
A baseline assessment of current practices and outcomes was undertaken in four important areas of supportive care; malnutrition and nutritional support, fever and neutropeni and treatment related mortality.
The results showed that the cause of death in the majority of patients (89%) who had died during treatment was treatment related (toxicity of treatment). This means that improved supportive care is needed.
The results also showed that only 15% of children who were diagnosed with a fever during neutropenia (low white blood cell count, reduced immunity) received antibiotics in the first hour after the onset of fever. We are currently preparing a programme aiming to improve the management of neutropenic fever.
Please find a summary of the baseline assessment and results in this short video.
Please find the video of the presentation of Dr Israels at the SIOP 2020 annual conference about the baseline assessment here (kindly create a CaseHippo user account to access the content free of charge)
SUCCOUR - Nursing programme
The SUCCOUR nursing programme is led by Glenn Mbah from Cameroon. A dedicated ‘SUCCOUR’ nurse was identified in each participating centre. This ‘SUCCOUR’ nurse is one of the ward, nursing team and is a role model and advocate for supportive care. Interactive monthly educational web meetings are arranged for the ‘SUCCOUR’ nurses. Thereafter the SUCCOUR nurse uses the same presentation to teach her team. An abstract to the SIOP 2020 annual meeting about this programme won the prize for ‘best SIOP Pediatric Oncology in Developing Countries (PODC) abstract’ for Africa.
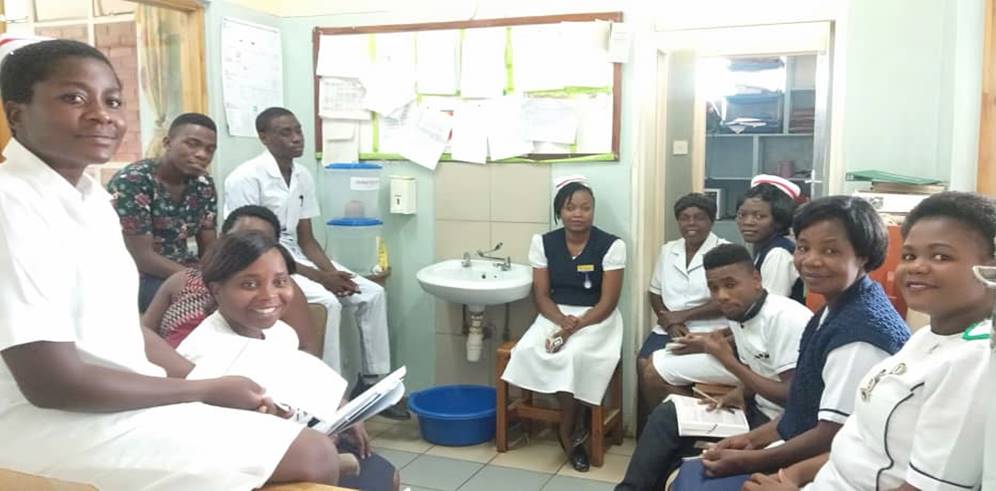
Pictures (4) of the nurse teaching on the ward.
Please find the link to Glenn Mbah’s presentation at the SIOP 2020 annual meeting here (kindly create a CaseHippo user account to access the content free of charge)
Nurses teaching on the ward
Results, impact and publications
T. Israels et al. Early death and treatment-related mortality: A report from SUCCOUR. Pediatr Blood Cancer 2021
T. Israels et al. Fever and neutropenia outcomes and areas for intervention: A report from SUCCOUR. Pediatr Blood Cancer 2021
The paper below is one of the adapted treatment guidelines of the Committee for Developing Countries (PODC) of SIOP, now the SIOP Global Health Network and provides some practical recommendations for supportive care in low- income countries.
Israels T., Renner L., Hendricks M. et al. SIOP PODC: Recommendations for supportive care of children with cancer in a low-income setting. Ped Blood Cancer 2013 2013 Jun;60(6):899-904.
https://siop-online.org/wp-content/uploads/2016/10/PBC-PODC-Supportive-Care-Guidelines.pdf